Overview of treatments for melanoma
This overview is intended to provide general information only and it is not a comprehensive treatment guide. Patients should discuss their treatment options, based on their individual circumstances, with their treating physicians.
Treatment options for melanoma have dramatically increased and improved over the last 10 years, including for advanced melanoma due to the discovery of novel targeted therapies and immunotherapies. Different treatments are considered based on the stage of the disease at diagnosis.
Melanoma begins with tissue damage triggered by excessive exposure to UV radiation and progresses through different stages. Its classification is known as TNM (Tumour, Node, Metastasis) staging. The thickness (depth) of the initial melanoma lesion is often a predictor of the clinical outcome. At the early stage it is localised in the skin (Stage 0-2) and can be successfully treated by excision (surgery). By Stage 3 the melanoma has reached the deeper skin layer and has spread to the lymph nodes and surrounding tissues and lymph nodes removal, with or without adjuvant treatment, is recommended. Advanced melanoma is described as Stage 4 and is characterised by metastasis, where the cancer has spread to tissues and organs throughout the body. Brain metastases can affect up to 50% of patients and their control is particularly important for their potential to greatly affect a patient’s quality of life.
Several treatment options, often used in combination, are now available and recently developed therapies have significantly improved the clinical outcome for patients experiencing this disease stage.
Surgical procedures used in the treatment of early stage melanoma are aimed at removing cancerous cells and surrounding tissues to reduce the risk of recurrence. These excision procedures are undertaken in day surgery. Larger wounds may require skin grafts. A lymph node close to the primary site is also tested at times if the melanoma is large. This is referred to as the sentinel node. If cancerous cells are detected in the sentinel node, more lymph nodes are removed and tested. This procedure is performed under general anaesthetic and requires hospital admission. Post-operative pain, stiffness and swelling (lymphoedema) are often experienced.
Surgery is also used for advanced melanoma and can involve the removal of the initial (primary) melanoma and metastases. The complexity and extent of the procedure will vary widely depending on the affected tissues and organs.
This treatment modality involves the use of X-rays, either to kill cancer cells which may not have been removed during surgery, and thus prevent the return of the primary melanoma, or to target existing metastases. Radiotherapy typically involves multiple sessions of a 20-30 minutes duration over several weeks, where radiation is targeted at affected areas. The number of radiotherapy treatments required depends on the size and location of the area being treated. The treatment is painless during administration. Recently developed RT techniques have increased the precision in targeting treatment using higher doses which can be aimed directly at the tumour, while sparing the surrounding healthy tissues. Stereotactic radiosurgery (SRS) is used in the treatment of brain metastases and uses a single, very high dose of radiation which targets the tumour by using three-dimensional coordinates. Stereotactic body RT (SBRT) is a similar technique used on parts of the body other than the brain and is administered at high doses in multiple fractions.
Tiredness, and skin reactions (redness, dryness, soreness, peeling, hair loss) within the treated area the most common side effects. Skin sensitivity to the sun may persist for extended periods. Nausea, loss of appetite and weight loss can also be experienced. Other side effects depend on the treatment site and duration of treatment. For example, radiation therapy to the brain may cause headaches, memory loss, seizures and hormonal changes when the pituitary gland is affected.
Chemotherapy is introduced when the cancer has spread beyond the initial (primary) melanoma. Chemotherapy drugs are administered intravenously, dissolved in a water solution, or orally as tablets. Chemotherapy works by attacking cells that are dividing quickly and therefore preferentially targets cancer cells, which replicate more quickly. Chemotherapy, however, also affects other rapidly dividing cells such as those found in the bone marrow (where new blood cells are made), the lining of the mouth and intestine, and hair follicles.
Chemotherapy is usually given in cycles and its side effects depend on the drug used, its dosage and administration regimen (frequency and overall duration of treatment). Common side effects are: fatigue, nausea and vomiting, diarrhoea or constipation, loss of appetite, hair loss, mouth sores, ease of bruising or bleeding, increased risk of infection, neuropathy (nerve pain, tingling, burning, heat/cold sensitivity). Side effects are usually temporary, and steps can be taken to prevent or reduce them, however the impact on a patient’s quality of life whilst undergoing chemotherapy can be considerable.
Chemotherapy is not as effective against melanoma as for other types of cancer. After the emergence of more effective and targeted therapies in the last decade, chemotherapy is less frequently used for the treatment of melanoma. It can, however, still play a role if more targeted therapies lose their effectiveness after prolonged use.
These are innovative, novel drugs, mostly used in the treatment of advanced or recurrent melanoma which has spread to other organs and can no longer be completely removed. They are administered orally as tablets or capsules once or twice a day and attack genetic changes (mutations) within melanoma cells, which facilitate the cancer’s growth and spread. Up to 80% of melanomas are estimated to present at least one genetic abnormality. Most targeted therapies are ‘cytostatic’ meaning they block cancer cell proliferation, rather than ‘cytotoxic’, such as chemotherapy, which kills tumour cells.
BRAF/MEK Inhibitors
The most common mutations targeted by these novel drugs are known as BRAF and MEK, which results in the synthesis of BRAF and MEK proteins which induce tumour growth. The drugs which target each of those mutations are BRAF and MEK inhibitors, respectively. The introduction of these drugs has substantially improved survival in patients with advanced melanoma presenting these mutations. In order to confirm whether a melanoma is likely to respond to these drugs, it needs to be tested for the presence of mutation by taking a sample of the cancer cells through a biopsy. For example, if a patient’s tumour is shown to contain the BRAF mutation, the patient is referred to as BRAF positive and can then be treated with a BRAF inhibitor.
Approximately half of all melanomas contain an altered form of the BRAF protein. BRAF and MEK inhibitors are often used in combination, as the combination therapy was found to work better than the single drugs alone. At the later stages of melanoma treatment effectiveness is generally measured by Progression-Free Survival (PFS), the length of time during and after treatment that a patient lives with the disease without getting worse.
Common side effects of BRAF inhibitors involve skin reactions (rash, itching, sensitivity to sunlight, skin thickening), headache, fever, nausea, joint pain and hair loss. Less common but serious side effects include heart rhythm alterations, liver problems, kidney failure, severe allergic reactions, eye disturbances, bleeding and increased blood sugar levels. Some patients can develop squamous cell skin cancer as a result of treatment. This is a treatable skin cancer, but regular skin monitoring is recommended after treatment.
Common side effects of MEK inhibitors include rash, nausea, swelling and sensitivity to sunlight. Rare but serious side effect reported include heart, lung or liver damage, blood clots, bleeding, muscle damage and skin infections. MEK inhibitors have been shown to also be effective in treating a further mutation detected in melanoma cells referred to as NRAS.
Less of the common side effects on the skin are generally observed when the combination of BRAF and MEK inhibitors is used. Most importantly the combination therapy has been shown to substantially improve the response rate, PFS and overall survival (OS), so that it has now become the standard of care for patients with advanced melanoma with the mutations which make it susceptible to these targeted therapies.
Some melanomas have activating mutations in the C-KIT gene. These involve most commonly mucosal melanomas (inside the mouth, for example, or in genital areas) and acral melanomas (which involve the palms of the hands, the soles of the feet and the skin under the nails). These mutations are targeted by other tyrosine kinase inhibitors (TKIs).
These are drugs which stimulate the body’s immune system to kill melanoma cells and are administered intravenously as a solution. Formulations for topical (localised) external use are available to treat small melanomas as they redevelop on the skin surface. It is estimated that about a third of patients with advanced melanoma will respond to immunotherapy. After an initial response melanoma can, however, become resistant to further therapy with these drugs. Various combinations of these drugs have been used and treatment protocols are rapidly evolving.
Immune checkpoint inhibitors are drugs referred to as monoclonal antibodies which target the ‘checkpoint’ proteins involved in healthy cell growth. Some melanomas have developed a mechanism to modulate these proteins, so as not to be recognised as malignant by the immune system. By turning off (inhibiting) these proteins on melanoma cells, these drugs help the immune system to attack them. There are two main new classes of drugs with this mechanism of action: PD-1 and CTLA-4 inhibitors. PD-1 and CTLA-4 are proteins, whose receptors are expressed on cancer cells and help suppress the immune response. By blocking these receptors, the immune system is stimulated to attack cancer cells.
PD-1 inhibitors boost the immune response to melanoma by blocking the PD-1 protein. These drugs are typically administered every few weeks over several months, with the duration of treatment depending on the clinical response.
Side effects include fatigue, cough, nausea, itching, skin rash, decreased appetite, constipation, joint pain, and diarrhea. Serious or even life-threatening side effect have been reported in the lungs, intestines, liver, hormone-making glands, kidneys, or other organs when the immune system starts attacking any of these organs. These side effects are rare.
Other promising drugs are CTLA-4 inhibitors which act by blocking the CTLA-4 protein on T cells and thus boost the immune response to melanoma. These are typically administered as an intravenous infusion every few weeks for a limited number of treatments. The most common side effects include fatigue, diarrhea, skin rash, and itching. As described for the PD-1 inhibitors, the immune system may attack other organs following treatment, which can lead to serious or life-threatening side effect in organs such as the intestine, liver, glands which secrete hormones, nerves, skin and eyes.
Interferons are cytokines, naturally occurring proteins which are part of the body’s immune response and are produced by white blood cells to fight viral and bacterial infections. Several interferons are available in Australia; however, they are not specifically approved for the treatment of melanoma. They are known to be used to prevent melanoma recurrence after excision.
Interleukins are endogenous proteins (ie found naturally within the body) belonging to the class referred to as cytokines, which are known to boost the immune system and can be used to treat melanoma. They are generally administered intravenously as a solution and can also be given as an injection under the skin. They can be used when other, more advanced therapies cease to be effective.
Oncolytic viruses are altered in a laboratory to make them effective in infecting and then killing cancer cells directly and through stimulating the immune response. They can be used to treat melanomas which affect the skin and lymph nodes when they cannot be excised through surgery. The modified virus is injected directly into the tumour, where it replicates and makes it shrink. Side effects are relatively mild and consist of flu-like symptoms and pain at the injection site.
Topical drugs used for the treatment of other skin conditions, including basal cell carcinoma, a less aggressive form of skin cancer, may be used for the treatment of early stage melanoma in areas where surgery is not recommended or desirable (such as the face). They generally act by stimulating a local immune response against cancer cells and are applied several times a week for up to 3 months. Skin reactions may occur during use.
Last revised August 2020
What to look for
An easy way to detect potentially harmful moles or lesions is to use the ABCDE guidelines.

Prevention and Early Dectection
Catching a melanoma early can save lives. Reducing your UV exposure can prevent melanoma.
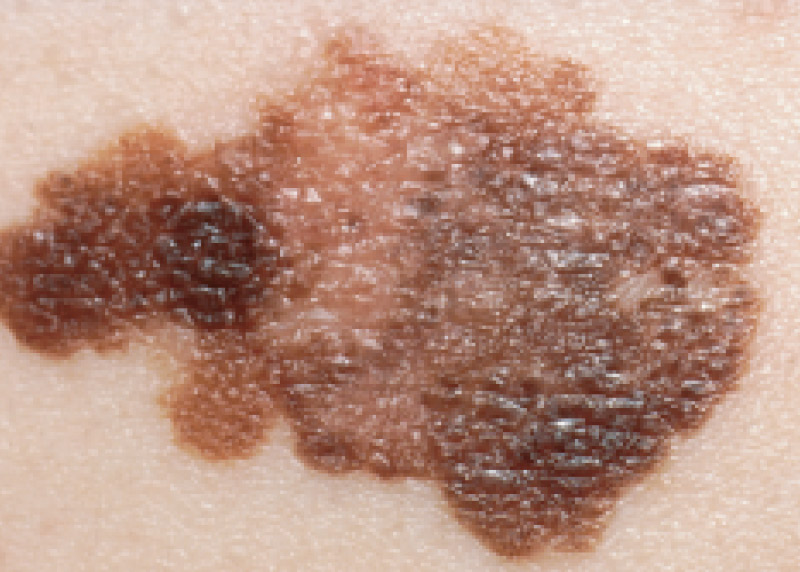
What is melanoma?
Find out more about melanoma and its prevalence in Australia.


